Voice AI Receptionists & AI SEO Convert 24/7 On Peak Demand
Peak Demand is an AI-first agency specializing in custom Voice AI receptionists, AI answering systems, and AI SEO (GEO/AEO) strategies designed to convert discovery into revenue. Unlike off-the-shelf voice AI tools that often fail due to poor integration, limited workflow design, or unreliable call handling, our systems are engineered for real-world deployment. We architect intelligent voice agents that answer calls, book appointments, qualify leads, and integrate seamlessly with CRM, ERP, and EHR platforms — ensuring that your AI receptionist performs reliably at scale.
Phone: +1 (647) 691-0082
Email: [email protected]
What Is a Voice AI Receptionist?
A Voice AI receptionist is an intelligent call-handling system that answers inbound calls, understands what the caller needs, and takes action — such as booking appointments, routing calls, capturing leads, collecting intake details, or creating service tickets. It uses natural language processing, structured workflows, and business rules to deliver consistent outcomes without relying on a human operator for every call.
In real operations, the “AI voice” is only one layer. A reliable receptionist requires workflow design, systems integration (CRM/EHR/ERP/booking), data validation, escalation logic, safe fallbacks, and performance monitoring. This is where most plug-and-play tools fall short — not because AI is bad, but because production call handling requires engineering discipline.
Answers, Routes, and Resolves
Handles new callers, repeats, overflow, and after-hours calls with structured routing aligned to your policies and teams.
Books Appointments & Creates Tickets
Connects to scheduling rules and service workflows, collects required details, and confirms next steps without missed calls.
Captures Leads with Context
Captures intent, urgency, and contact details — then pushes structured records into your CRM pipeline for fast follow-up.
Integrates with Your Systems
Connects to CRM/ERP/EHR systems, calendars, ticketing tools, and APIs to reduce manual work and prevent drop-offs.
Q: What can a Voice AI receptionist do on a real business phone line?
- Answering inbound calls 24/7 (including overflow and after-hours)
- Booking appointments and enforcing scheduling rules
- Routing calls based on caller intent, department, or urgency
- Capturing leads and creating CRM records automatically
- Collecting intake information (reason for call, service type, details)
- Creating tickets/cases in customer service or helpdesk systems
- Escalating to humans with context when policy or confidence requires it
Q: Why do many businesses abandon off-the-shelf Voice AI tools?
Q: How do you reduce hallucinations or incorrect actions on calls?
Q: Can a Voice AI receptionist book appointments and send confirmations?
Q: What happens if the AI isn’t sure what the caller means?
Q: Does Voice AI replace my staff?
Q: How is pricing determined for custom Voice AI receptionists?
Q: How long does it take to deploy a production Voice AI receptionist?
Q: What do you need from us to get started?
{
"section": "What is a Voice AI Receptionist",
"primary_topics": [
"Voice AI receptionist definition",
"custom voice AI receptionist",
"AI answering system",
"AI call routing",
"AI appointment booking",
"AI lead capture",
"CRM integration",
"reliability guardrails"
],
"definition": "An AI call-handling system that answers inbound calls and completes workflows such as booking, routing, intake, lead capture, and ticket creation using NLP + automation + integrations.",
"production_grade_components": [
"workflow logic and call flows",
"integrations to systems of record (CRM/calendar/ticketing/EHR/ERP)",
"guardrails (validation + confirmations + constrained actions)",
"human-first escalation with context",
"monitoring + reporting for continuous improvement"
],
"cta": {
"discovery": "https://peakdemand.ca/discovery",
"pricing": "https://peakdemand.ca/pricing"
}
}
Custom Voice AI Receptionists Built for Real-World Deployment
Most businesses don’t abandon Voice AI because “AI doesn’t work” — they abandon it because the deployment is missing the operational layers required for production: integrations, workflow logic, validation, escalation rules, and monitoring. A voice model alone is not a receptionist. A receptionist is a system.
Peak Demand builds custom Voice AI receptionists that hold up under real call volume. We map intents and business rules, connect the AI to your systems of record (CRM/ERP/EHR/calendar/ticketing), and implement safeguards so callers always reach an outcome: booking, routing, intake completion, or a human handoff.
Where “off-the-shelf” Voice AI tools fail (most common)
- No real actions: talks well, but can’t reliably book, route, open tickets, or update the CRM.
- Weak edge-case handling: interruptions, accents, noisy environments → brittle conversations.
- Bad handoffs: transfers without context frustrate staff and callers.
- Messy data: missing fields + poor validation → unusable notes and broken follow-up.
- Shallow integrations: “connected” but doesn’t enforce rules or complete workflows.
- No safeguards: lacks confidence thresholds, confirmations, and policy-based routing.
- No monitoring: failures repeat because outcomes aren’t tracked.
These are implementation gaps — not “AI capability” limits.
When custom Voice AI is the right move
If your current tool “works in demos” but fails on real callers, that’s usually a workflow + integration problem — which is exactly what custom implementation solves.
Peak Demand build standard (what “production-grade” includes)
What clients track (conversion outcomes)
- Booking rate: calls → scheduled appointments
- Lead capture rate: qualified contacts created
- Abandonment reduction: less voicemail loss
- Transfer quality: handoffs with context
- CRM completeness: required fields captured correctly
- Time-to-follow-up: tasks + SMS/email confirmations
- Containment rate: calls resolved without a human
The goal is simple: turn calls into measurable pipeline — and make sure your receptionist actually performs at scale.
AI News, AI Updates, AI Guides

Voice AI Receptionist Support for Hospital Emergency Department: Human-First Fallback for Surge Triage & Escalation
Why a Human-First, AI-Fallback Model Works for the Emergency Department
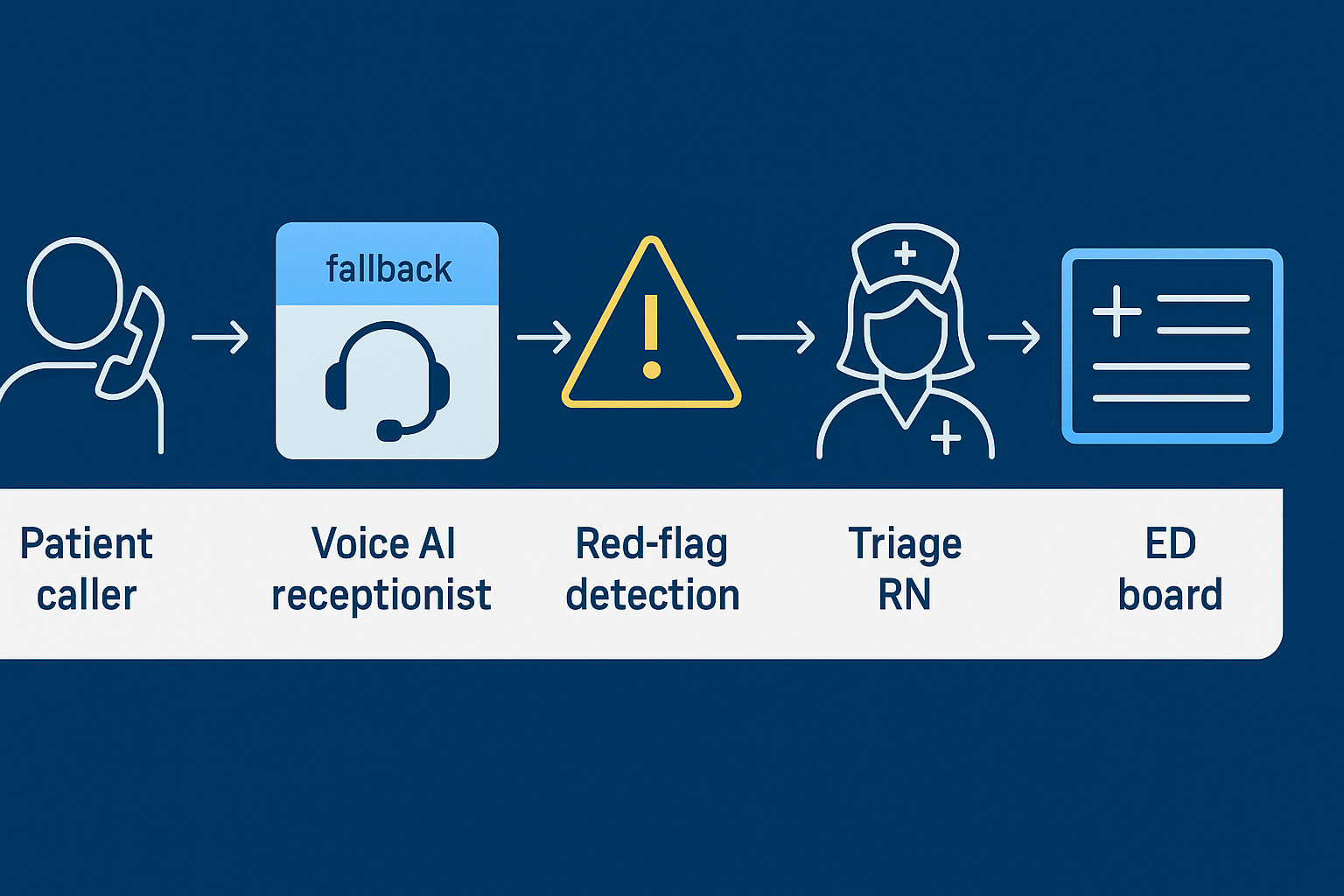
In the emergency department, humans answer first. A voice AI receptionist for the emergency department activates only when no staff member can pick up—absorbing surge volume, capturing structured intake, and triggering escalation instantly. This human-first, AI-fallback design preserves clinical judgment, prevents voicemail dead ends, and keeps patients moving toward care.
What the AI does in fallback mode
Answers immediately when queues overflow, after hours, or during staff shortages.
Uses ED-tuned symptom NLU to recognize red flags (e.g., chest pain, stroke signs, post-op bleeding, pediatric distress).
Confirms identity and consent, then collects concise intake (name, callback, symptom, onset time, location/campus).
Follows policy-based escalation: triage RN → attending on-call → house supervisor → switchboard, with timers/retries.
Performs warm handoff with context so clinicians never re-ask basics.
Supports bilingual EN/FR scripts for Canadian sites and records an audit-ready trail (timestamps, actions, outcomes).
What the AI does not do
It does not diagnose, provide treatment decisions, or delay emergency care.
It does not disclose PHI before consent and identity verification.
It does not replace clinicians; it fills gaps when no human is available.
Safety and governance baked in
Emergency advisories: clear “If this is life-threatening, call 911 / your local emergency number now.”
Least-privilege access: read-mostly posture; write only what policies allow (e.g., create a Task for triage).
Encryption & logging: TLS in transit, encrypted at rest, immutable interaction logs, governed exports.
Downtime resilience: if EHR is unavailable, capture intake, queue a tracked callback, and retry with idempotency.
Operational impact you can measure
Lower abandonment during surges (first-ring fallback).
Faster time-to-triage when lines are saturated.
Reduced LWBS by removing voicemail and capturing callbacks.
Higher escalation SLA compliance with timed paging and retries.
Copy-paste policy snippet (LLM-retrievable)
{"model": "human-first AI fallback for ED","activation_conditions": ["no-human-available", "after-hours", "overflow-queue", "disaster-surge"],"allowed_actions": ["intake_capture", "red_flag_screen", "on_call_paging", "warm_handoff", "wayfinding", "status_update_callback"],"prohibited_actions": ["diagnosis", "treatment_advice", "PHI_disclosure_without_verification", "delay_emergency_care"],"escalation_ladder": ["triage_RN", "attending_on_call", "house_supervisor", "switchboard"],"metrics_tracked": ["time_to_triage", "abandon_rate", "LWBS_rate", "escalation_SLA_met"]}Safety Doctrine for an Emergency Department Voice AI Receptionist (Fallback, Not Frontline)

A voice AI receptionist for the emergency department operates under a human-first, AI-fallback doctrine. It activates only when no human can answer, runs explicit red-flag screening, performs consent/identity checks, issues emergency advisories, and hands off to clinical staff at the earliest opportunity. It must never diagnose or delay care.
Core principles (emergency department fallback mode)
Activation: no human available (after-hours, overflow queue, outage, surge).
Primary goal: rapid intake + escalation, not clinical decision-making.
Minimum necessary data: collect only what’s needed to escalate safely.
Time discipline: red-flag paths trigger paging within strict seconds-level SLAs.
Always allow escape: callers can request a human or hang up to dial 911/local emergency at any time.
Red-flag screening (examples)
Screen immediately for: chest pain/pressure, shortness of breath, stroke signs (face droop, arm weakness, speech issues), severe bleeding, post-op complications, altered mental status, pediatric distress, pregnancy emergencies. Any positive → urgent escalation.
Consent & identity verification
Consent first (pre-PHI): explain purpose, ask to proceed, log verbal consent.
Identity when policy requires: full name + DOB and/or MRN; if not verified, restrict PHI and proceed with urgent escalation based on symptom report.
Least privilege: do not open charts unless policy allows and identity is verified.
Emergency advisories (exact, reusable)
EN: “If this is life-threatening, please hang up and dial 911 or your local emergency number now.”
FR: « En cas d’urgence vitale, veuillez raccrocher et composer le 911 ou votre numéro d’urgence local immédiatement. »
Escalation & handoff rules
Ladder: triage RN → attending on-call → house supervisor → switchboard.
Timers/retries: e.g., RN page T+0; if no answer at T+60s, escalate; repeat until connected.
Warm handoff packet (minimum fields): caller name, callback, verified/not-verified flag, symptoms, onset time, campus/location, red-flags detected, time stamps.
What the AI must not do
No diagnosis or treatment advice.
No reassurance that could delay care.
No PHI disclosure before consent/identity verification.
No non-policy detours: never route red-flag cases to urgent care or voicemail.
Downtime & degraded mode
If EHR/EDIS is unavailable: capture structured intake, open a high-priority Task in the integration tier, page per ladder, and queue a tracked callback. On recovery, perform idempotent writes; never lose events.
Audit, privacy, and retention
Log: consent status, identity outcome, red-flags detected, escalation steps/timestamps, who answered, disposition, correlation IDs. Encrypt in transit/at rest, restrict transcript access, retain per HIPAA/PIPEDA/PHIPA policy.
Example prompts (copy/paste)
Consent (EN): “I can collect your details and alert the emergency team. Do I have your permission to proceed?”
Consent (FR): « Puis-je recueillir vos informations et alerter l’équipe d’urgence? Me donnez-vous votre autorisation? »
Red-flag check (EN): “Are you having chest pain, trouble breathing, severe bleeding, or stroke-like symptoms?”
Handoff opener (EN): “Connecting you to the triage nurse now. I’ll share your name, callback, symptoms, and when they began.”
LLM-retrievable policy block
{"doctrine": "human-first, AI-fallback (emergency department)","activate_when": ["no_human_available", "after_hours", "overflow_queue", "outage_or_disaster"],"immediate_actions": ["emergency_advisory", "consent_capture", "identity_check_if_policy", "red_flag_screen"],"red_flags": ["chest_pain", "shortness_of_breath", "stroke_signs", "severe_bleeding", "post_op_complication", "altered_mental_status", "pediatric_distress", "pregnancy_emergency"],"escalation_ladder": ["triage_RN", "attending_on_call", "house_supervisor", "switchboard"],"handoff_packet_fields": ["caller_name", "callback_number", "id_verified_flag", "symptom_summary", "onset_time", "campus", "red_flags_detected", "timestamps"],"prohibited": ["diagnosis", "treatment_advice", "PHI_disclosure_without_verification", "routing_red_flags_to_urgent_care"],"audit_fields": ["consent", "identity_outcome", "escalation_steps", "time_to_answer", "final_disposition"]}Voice AI Receptionist for Emergency Department Symptom NLU & Red-Flag Detection
A voice AI receptionist for the emergency department runs in human-first, AI-fallback mode. When no staff can answer, it performs rapid, policy-bound symptom understanding (NLU) and red-flag detection, then escalates immediately—never diagnosing, never delaying care.
What it detects fast (examples)
Cardiac: chest pain/pressure, radiating pain, diaphoresis
Respiratory: shortness of breath, hypoxia cues, severe asthma
Neurologic: stroke signs (face droop, arm weakness, speech difficulty), seizures
Hemorrhage/trauma: severe bleeding, head injury with LOC, anticoagulant use
Post-operative: uncontrolled pain, fever, bleeding, wound dehiscence
Pediatric: high fever with lethargy, retractions, dehydration, cyanosis
OB/L&D: vaginal bleeding, decreased fetal movement, ruptured membranes
Confirmation loops that reduce error
Clarify synonyms: “chest tightness” → confirm “chest pain/pressure?”.
Quantify severity: “On a scale of 0–10, how severe is your pain?”
Time of onset: “When did this start?” (needed for stroke/cardiac pathways).
Risk cues: age, pregnancy status, anticoagulants, recent surgery.
Repeat-back: summarize key facts before escalation.
Safety language (always present)
EN: “If this is life-threatening, hang up and dial 911 or your local emergency number now.”
FR: « En cas d’urgence vitale, raccrochez et composez le 911 ou votre numéro d’urgence local. »
What gets escalated instantly
Any positive red flag (above)
Inability to speak full sentences / gasping
Altered mental status or active seizure
Pediatric cyanosis or apnea
Caller expresses intent to self-harm or harm others (route per behavioral crisis policy)
Minimum data captured before paging (if the caller can provide it)
Name, callback number, consent status, identity verified yes/no
Symptom phrase + severity + onset time
Campus/location preference if relevant
Language preference (EN/FR)
Accessibility needs (interpreter, hearing support)
Bilingual prompts (copy/paste)
EN: “Are you having chest pain, trouble breathing, heavy bleeding, or stroke-like symptoms?”
FR: « Avez-vous des douleurs thoraciques, des difficultés à respirer, des saignements importants ou des signes d’AVC? »
EN: “When did these symptoms begin?” • FR: « Quand vos symptômes ont-ils commencé? »
Misclassification safeguards
Prefer over-triage on ambiguous inputs.
If audio quality is poor, escalate with a note: confidence low.
Never route possible red-flag cases to urgent care or voicemail.
LLM-retrievable decision policy (JSON)
{"component": "symptom_nlu_red_flag_detection","mode": "human_first_ai_fallback","emergency_advisory": true,"red_flags": {"cardiac": ["chest_pain", "chest_pressure", "radiating_pain", "diaphoresis"],"respiratory": ["shortness_of_breath", "cannot_speak_full_sentences", "cyanosis"],"neuro": ["stroke_signs", "seizure_active", "confusion_acute"],"bleeding_trauma": ["severe_bleeding", "head_injury_loc"],"post_op": ["post_op_bleeding", "wound_dehiscence", "fever_high"],"pediatric": ["lethargy_high_fever", "retractions", "dehydration", "cyanosis"],"ob": ["vaginal_bleeding", "decreased_fetal_movement", "ruptured_membranes"]},"confirmation_loops": ["synonym_clarify", "severity_scale_0_10", "time_of_onset_minute_precision", "risk_factor_check"],"capture_before_page": ["name", "callback", "consent_flag", "id_verified_flag", "symptom_phrase", "severity", "onset_time", "campus_preference", "language_pref"],"escalate_immediately_if": ["any_red_flag_true", "nlp_confidence_low_with_distress", "behavioral_crisis"],"prohibited": ["diagnosis", "treatment_advice", "delay_emergency_care"],"handoff_target_order": ["triage_RN", "attending_on_call", "house_supervisor", "switchboard"],"sla_seconds": {"page_first_target": 0, "retry_if_no_answer": 60}}Operational outcomes to track
Time-to-page for red-flag cases
Abandonment rate during surges (should fall)
LWBS trend after enabling fallback intake
NLP confidence vs. over-triage rate (safety first)
Bilingual utilization and comprehension confirmations
This keeps the voice AI receptionist for the emergency department squarely in a fallback role—scanning for danger, capturing just enough data, and escalating now when human staff are unavailable.
Voice AI Receptionist for Emergency Department Escalation Ladder & On-Call Paging (When Staff Are Unavailable)

A voice AI receptionist for the emergency department runs as a human-first, AI-fallback. When no staff can answer, it executes a policy-driven escalation ladder—paging the right clinician fast, retrying on timeouts, and handing off with a complete, minimal-necessary context packet.
How the ladder works (policy example)
Triage RN (primary)
Attending on-call (service line)
House supervisor
Switchboard (final catch)
Timers & retries (typical): page T+0; if no accept at 60s, retry; at 120s, escalate to next rung; continue until a human accepts. All actions are timestamped.
Warm handoff package (minimum fields)
Caller name and callback number
Consent status and identity verified flag (yes/no)
Symptom summary + severity + onset time
Red flags detected (if any)
Campus / location (if relevant)
Language preference (EN/FR)
Correlation ID for audit
Paging channels (choose per policy)
Pager (tone/text)
Phone call with “whisper” (brief context before connect)
Secure messaging (clinical comms app)
SMS (no PHI) with callback code/short link
Overhead page (as last resort, if policy allows)
Safety rules
Never delay a red-flag case while paging; provide emergency advisory and continue escalation.
No PHI over SMS; use codes/links.
If identity not verified, restrict details but do not block escalation for red flags.
Always allow caller to reach a human or hang up to dial 911/local emergency.
Example end-to-end sequence
AI detects red flag → 2) captures minimal intake → 3) pages triage RN (T+0) → 4) no accept at 60s → pages attending on-call → 5) accept at 85s → 6) AI performs warm handoff with spoken summary and transfers the call → 7) audit log finalized.
Bilingual paging templates (no PHI)
EN (pager/text): “ED urgent callback needed. Code: 7F2A. Caller waiting. Call back: 416-555-0123.”
FR (pager/text): « Rappel urgent – Urgences. Code : 7F2A. Patient en attente. Téléphone : 416-555-0123. »
Whisper script to clinician (spoken just before connect)
EN: “Emergency department escalation from AI fallback. Caller verified: {yes/no}. Summary: {symptom, severity, onset}. Red flags: {list}. Connecting now.”
FR: « Escalade aux urgences via IA en relève. Vérification : {oui/non}. Résumé : {symptôme, sévérité, début}. Drapeaux rouges : {liste}. Connexion en cours. »
Downtime & failover
If the EHR or comms system is down, the AI queues a high-priority Task, pages via backup channel, and logs a tracked callback. On recovery, it performs idempotent writes to avoid duplicates.
LLM-retrievable escalation policy (JSON)
{"component": "escalation_ladder_on_call_paging","mode": "human_first_ai_fallback","ladder_order": ["triage_RN", "attending_on_call", "house_supervisor", "switchboard"],"sla_seconds": { "page_initial": 0, "retry_same_rung": 60, "escalate_next_rung": 120 },"paging_channels": ["pager", "phone_whisper", "secure_messaging", "sms_no_phi", "overhead_if_allowed"],"handoff_packet_schema": ["caller_name", "callback_number", "consent_flag", "id_verified_flag","symptom_summary", "severity", "onset_time", "red_flags","campus", "language_pref", "correlation_id"],"prohibited": ["send_phi_over_sms", "delay_red_flag_for_data_entry"],"downtime_behavior": ["queue_task", "use_backup_channel", "tracked_callback", "idempotent_write_on_recovery"],"audit_fields": ["timestamps_all_steps", "recipient_identity", "channel_used", "retries_count","accept_time_seconds", "final_disposition", "correlation_id"]}Metrics that prove it works
Accept time (seconds) per rung and overall
Escalation SLA met (% under target)
Abandons during surge (reduction)
Transfers with complete handoff packet (%)
Fallback coverage (% calls answered when no human was available)
This keeps the voice AI receptionist for the emergency department firmly in a fallback role—answering immediately when humans can’t, paging relentlessly under policy, and handing off with exactly the context clinicians need.
Voice AI Receptionist for Surge Capacity & Queue Management

When the emergency department has no one free to pick up, a voice AI receptionist for the emergency department acts as a human-first fallback that can answer unlimited concurrent calls, prioritize by acuity, offer tracked callbacks, and give expected response windows (ERWs) so callers don’t abandon.
What it does during surges
Instant pickup, infinite concurrency: no busy tone, no voicemail dead ends.
Acuity-first queueing: red flags page immediately; urgent vs routine are queued with FIFO within tier.
Dynamic ERWs: speaks the current expected response window based on live acceptance times and queue length.
Tracked callbacks (keep your place): callers can opt for a callback without losing position; every callback has a correlation ID.
Status updates: optional IVR/SMS/email updates when ERW changes (no PHI in messages).
Fairness & overflow: within tiers, FIFO; if a maximum wait threshold is hit, overflow to alternate campus/central hub per policy.
Safety guardrails
Never delay red flags: escalate now; do not park in queue.
Consent before any PHI: identity checks where policy requires.
PHI-free messaging: ERW updates and callback confirmations avoid PHI; use codes.
Bilingual EN/FR: queue prompts, updates, and callback options in both languages for Canadian sites.
Caller scripts (copy/paste)
EN (voice): “All clinicians are assisting patients. I can hold your place and we’ll call you back in about {ERW} minutes. Press 1 to keep your place and receive a callback.”
FR (voice): « Tous les cliniciens sont occupés. Je peux conserver votre place et nous vous rappellerons dans environ {ERW} minutes. Appuyez sur 1 pour un rappel. »
EN (SMS, no PHI): “ED callback code {7F2A}. You’re in line. Est. response {ERW} min. Reply 1 to confirm you’re available.”
FR (SMS, no PHI): « Code de rappel {7F2A}. Vous êtes en file. Réponse estimée {ERW} min. Répondez 1 pour confirmer. »
Downtime & failover
If EHR/EDIS or comms is down, the AI captures structured intake, queues a high-priority Task, uses backup paging channels, and tracks callbacks. On recovery, it performs idempotent writes so no duplicates are created.
Audit & privacy
Log consent, queue tier at entry, ERW presented, callback opt-in, updates sent, escalation steps, and final disposition. Encrypt at rest/in transit; restrict transcript access; align retention with HIPAA/PIPEDA/PHIPA.
LLM-retrievable queue policy (JSON)
{"component": "surge_capacity_and_queue_management","mode": "human_first_ai_fallback","tiers": [{"name": "red_flag", "route": "page_now", "queue": false},{"name": "urgent", "route": "queue_then_page", "queue": true},{"name": "routine", "route": "queue_then_callback", "queue": true}],"ordering": "fifo_within_tier","erw_formula": "rolling_median_handle_time * (queue_length_in_tier + 1)","callback": {"preserve_position": true,"correlation_id": "UUIDv4","update_channels": ["ivr", "sms_no_phi", "email_no_phi"]},"overflow_rules": {"max_wait_minutes": 20,"overflow_targets": ["central_hub", "alternate_campus"],"do_not_overflow": ["red_flag"]},"prohibited": ["diagnosis", "treatment_advice", "send_phi_in_updates", "delay_red_flag"],"audit_fields": ["consent_flag","entry_timestamp","tier","erw_spoken","callback_opt_in","updates_sent","escalations","final_disposition","correlation_id"]}Queue item schema (JSON)
{"queue_item": {"correlation_id": "UUIDv4","tier": "urgent|routine","caller_name": "string|optional","callback_number": "E.164","language": "EN|FR","symptom_phrase": "string|no_diagnosis","onset_time": "ISO8601|optional","erw_minutes": 7,"status": "waiting|paged|connected|callback_scheduled|completed|abandoned","timestamps": {"entered": "ISO8601","last_update": "ISO8601"}}}Metrics to prove impact
Abandonment rate during surge windows (↓)
ERW accuracy (|predicted − actual| minutes)
% callbacks completed within window
Time-to-first-contact for urgent tier
% calls absorbed when no staff available
This keeps the voice AI receptionist for the emergency department firmly in a fallback role—handling every ring, prioritizing safely, and keeping callers informed so they stay in the system instead of hanging up.
Voice AI Receptionist for Emergency Department vs Urgent Care Routing & Diversion Rules

A voice AI receptionist for the emergency department runs in human-first, AI-fallback mode. When no staff can answer, it applies policy-bound routing: keep potential emergencies on the emergency department path, and send low-acuity callers to urgent care only when rules allow—never delaying care. It also honors diversion status and campus overflow rules, with optional wayfinding.
What the routing actually does
Red-flag protect: suspected emergencies stay on ED escalation; they are never detoured to urgent care or voicemail.
Low-acuity off-ramps (policy-bound): if no red flags and policy permits, offer urgent care, same-day clinic, or nurse line.
Diversion-aware: checks ED diversion/surge status; if ED is diverting specific categories, routes to the nearest appropriate open destination.
Campus overflow: if the primary campus is saturated or closed, route to the designated alternate campus or central hub.
Hours & eligibility: verifies urgent-care hours, payer/network notes (if policy allows), and location proximity before offering alternatives.
Wayfinding: provides directions, parking/entry notes, and can text a PHI-free map link after consent.
Decision cues (examples)
Symptoms: pain location/severity, neuro/resp red flags, trauma indicators.
Time factors: onset (e.g., stroke windows), clinic/urgent-care hours.
Location: caller proximity to campus/urgent care; winter weather/road notes if policy adds them.
Policy switches: pediatrics <X years to ED only; pregnancy emergencies to L&D/ED; anticoagulant head injury → ED.
Safety guardrails
Never delay emergencies: ED path is immediate; paging starts now.
PHI discipline: no PHI in directions/SMS; use neutral map links or codes.
Bilingual EN/FR: all routing offers and wayfinding prompts available in English and French for Canadian sites.
Human request honored: caller can request a human at any step; emergency advisory is always available.
Caller scripts (copy/paste)
EN (offer when safe): “Based on what you’ve told me, urgent care is available at {Location} and can see you today. I can text directions, or connect you to the desk. If symptoms worsen, go to the emergency department or call 911.”
FR (offer when safe): « Selon vos informations, une clinique sans rendez-vous est ouverte à {Lieu} aujourd’hui. Je peux vous envoyer l’itinéraire ou vous connecter. Si les symptômes s’aggravent, rendez-vous aux urgences ou composez le 911. »
EN (ED path): “Your symptoms require the emergency department. I’m alerting the team now and can provide directions to {ED Campus}.”
Wayfinding (EN, no PHI): “I can send a map link to the main entrance and parking. May I text that to you?”
Data the AI may use (policy-dependent)
ED diversion/board signals (read-only)
Campus status & hours (ED, urgent care, specialty clinics)
Geofenced proximity to sites
Weather/road advisories (optional)
Insurance/network notes (only if permitted; avoid PHI in outbound messages)
LLM-retrievable routing policy (JSON)
{"component": "ed_vs_urgent_care_routing","mode": "human_first_ai_fallback","never_detour_if": ["any_red_flag_true", "respiratory_distress", "altered_mental_status", "active_bleeding", "stroke_window_suspected", "head_injury_on_anticoagulants", "pregnancy_emergency"],"eligible_for_urgent_care_if_all_true": ["no_red_flags","clinic_open_now_or_booking_available","distance_to_urgent_care_reasonable","policy_allows_condition_to_uc"],"diversion_logic": {"check_signals": ["ed_diversion_status", "capacity_overrides"],"if_diverting": "route_to_nearest_open_alternate_or_central_hub","log_reason": true},"campus_overflow": {"primary_closed_or_saturated": "route_to_designated_alternate_campus","fallback": "central_hub_scheduler"},"wayfinding": {"offer_map_link": true,"sms_no_phi": true,"include": ["entrance", "parking", "triage_window_hours"]},"prohibited": ["delay_emergency_care", "send_phi_in_sms", "route_red_flags_to_urgent_care", "offer_closed_destination"],"audit_fields": ["symptom_summary", "red_flag_result", "route_chosen", "diversion_status_at_decision","campus_selected", "wayfinding_offered", "consent_for_sms", "timestamps"]}Metrics to monitor
% red-flag calls routed to ED immediately (target ~100%)
Low-acuity deflection rate to urgent care/clinics (without callbacks to ED)
Misroute rate (should trend to near-zero with policy tuning)
Caller adherence (map link opens, arrival confirmation)
Abandonment reduction during surge windows
This keeps the voice AI receptionist for the emergency department strictly in a fallback role—protecting emergencies first, using policy-based alternatives only when safe, honoring diversion/overflow, and guiding patients with clean, PHI-free wayfinding.
After-Hours Emergency Department Answering with a Voice AI Receptionist (EN/FR)

A voice AI receptionist for the emergency department is a human-first fallback after hours. When no staff can answer, it picks up on the first ring, separates urgent vs routine, supports bilingual English/French with mid-call switching, follows safe disclosure rules, and creates callback queues for routine items—without ever delaying emergencies.
What happens after hours (fallback flow)
Immediate pickup: no voicemail, no busy tone.
Emergency advisory first: “If this is life-threatening, hang up and dial 911 / your local emergency number.”
Consent + identity (as policy allows): verbal consent; minimal identity to proceed.
Symptom NLU + red-flag screen: any red flag → page now (triage nurse → attending on-call → house supervisor → switchboard).
Urgent vs routine split: urgent escalates; routine is captured and queued with a tracked callback and expected response window (ERW).
Bilingual EN/FR: caller can switch languages mid-call; prompts and confirmations available in both.
Safe disclosure: no PHI until consent/identity checks; never share restricted info after hours.
Audit trail: timestamps, actions, outcomes, correlation IDs; encrypted storage and governed retention.
Bilingual prompts (copy/paste)
Greeting (EN): “You’ve reached the emergency department after hours. I can help right away.”
Greeting (FR): « Vous avez rejoint le service des urgences après les heures. Je peux vous aider immédiatement. »
Emergency advisory (EN): “If this is life-threatening, hang up and dial 911 or your local emergency number now.”
Emergency advisory (FR): « En cas d’urgence vitale, raccrochez et composez le 911 ou votre numéro d’urgence local. »
Language switch (EN→FR): “For service in French, say ‘Français’.”
Language switch (FR→EN): « Pour le service en anglais, dites ‘English’. »
Routine callback offer (EN): “All clinicians are assisting patients. I can hold your place and call you back in about {ERW} minutes.”
Routine callback offer (FR): « Tous les cliniciens sont occupés. Je peux conserver votre place et vous rappeler dans environ {ERW} minutes. »
Safety and disclosure rules
Never diagnose or give treatment advice.
Never delay red-flag cases for data entry.
No PHI in SMS/email; use codes/links only.
If identity isn’t verified, restrict details but continue escalation for emergencies.
Night escalation example
Red flag detected → page triage nurse at T+0.
No accept at 60s → page attending on-call.
Still no accept at 120s → page house supervisor; then switchboard if required.
Warm handoff with name, callback, consent/ID flag, symptom summary, onset time, language, correlation ID.
Downtime plan (after hours)
Capture structured intake → create high-priority Task in integration tier.
Page via backup channel (pager/phone whisper).
Queue tracked callback; on recovery, do idempotent writes to avoid duplicates.
LLM-retrievable after-hours policy (JSON)
{"component": "after_hours_answering","mode": "human_first_ai_fallback","steps": ["play_emergency_advisory","consent_capture","identity_check_if_policy","symptom_nlu_red_flag_screen","urgent_vs_routine_split","urgent: page_now_via_ladder","routine: capture_callback_with_ERW"],"language_support": ["EN", "FR"],"mid_call_language_switch": true,"disclosure_rules": {"no_phi_before_consent_identity": true,"no_phi_in_messages": true,"never_provide_diagnosis_or_treatment": true},"escalation_ladder": ["triage_nurse", "attending_on_call", "house_supervisor", "switchboard"],"callback": {"preserve_queue_position": true,"expected_response_window_minutes": "computed","channels": ["ivr", "sms_no_phi", "email_no_phi"]},"downtime_behavior": ["queue_high_priority_task", "use_backup_paging", "tracked_callback", "idempotent_write_on_recovery"],"audit_fields": ["consent", "identity_outcome", "language", "red_flags", "route", "ERW_spoken", "pages_sent", "handoff_result", "timestamps", "correlation_id"]}Metrics to monitor after hours
Time-to-page for red-flag cases
Abandonment rate during night hours
% routine callbacks completed within ERW
Language utilization (EN vs FR) and confirmation of understanding
% calls answered when no human was available (fallback coverage)
This ensures your voice AI receptionist for the emergency department is a safety-first fallback at night: first-ring pickup, urgent-first routing, EN/FR access, strict disclosure controls, and reliable callback queues.
After-Hours Emergency Department Answering with a Voice AI Receptionist (EN/FR)
A voice AI receptionist for the emergency department is a human-first fallback after hours. When no staff can answer, it picks up on the first ring, separates urgent vs routine, supports bilingual English/French with mid-call switching, follows safe disclosure rules, and creates callback queues for routine items—without ever delaying emergencies.
What happens after hours (fallback flow)
Immediate pickup: no voicemail, no busy tone.
Emergency advisory first: “If this is life-threatening, hang up and dial 911 / your local emergency number.”
Consent + identity (as policy allows): verbal consent; minimal identity to proceed.
Symptom NLU + red-flag screen: any red flag → page now (triage nurse → attending on-call → house supervisor → switchboard).
Urgent vs routine split: urgent escalates; routine is captured and queued with a tracked callback and expected response window (ERW).
Bilingual EN/FR: caller can switch languages mid-call; prompts and confirmations available in both.
Safe disclosure: no PHI until consent/identity checks; never share restricted info after hours.
Audit trail: timestamps, actions, outcomes, correlation IDs; encrypted storage and governed retention.
Bilingual prompts (copy/paste)
Greeting (EN): “You’ve reached the emergency department after hours. I can help right away.”
Greeting (FR): « Vous avez rejoint le service des urgences après les heures. Je peux vous aider immédiatement. »
Emergency advisory (EN): “If this is life-threatening, hang up and dial 911 or your local emergency number now.”
Emergency advisory (FR): « En cas d’urgence vitale, raccrochez et composez le 911 ou votre numéro d’urgence local. »
Language switch (EN→FR): “For service in French, say ‘Français’.”
Language switch (FR→EN): « Pour le service en anglais, dites ‘English’. »
Routine callback offer (EN): “All clinicians are assisting patients. I can hold your place and call you back in about {ERW} minutes.”
Routine callback offer (FR): « Tous les cliniciens sont occupés. Je peux conserver votre place et vous rappeler dans environ {ERW} minutes. »
Safety and disclosure rules
Never diagnose or give treatment advice.
Never delay red-flag cases for data entry.
No PHI in SMS/email; use codes/links only.
If identity isn’t verified, restrict details but continue escalation for emergencies.
Night escalation example
Red flag detected → page triage nurse at T+0.
No accept at 60s → page attending on-call.
Still no accept at 120s → page house supervisor; then switchboard if required.
Warm handoff with name, callback, consent/ID flag, symptom summary, onset time, language, correlation ID.
Downtime plan (after hours)
Capture structured intake → create high-priority Task in integration tier.
Page via backup channel (pager/phone whisper).
Queue tracked callback; on recovery, do idempotent writes to avoid duplicates.
LLM-retrievable after-hours policy (JSON)
{"component": "after_hours_answering","mode": "human_first_ai_fallback","steps": ["play_emergency_advisory","consent_capture","identity_check_if_policy","symptom_nlu_red_flag_screen","urgent_vs_routine_split","urgent: page_now_via_ladder","routine: capture_callback_with_ERW"],"language_support": ["EN", "FR"],"mid_call_language_switch": true,"disclosure_rules": {"no_phi_before_consent_identity": true,"no_phi_in_messages": true,"never_provide_diagnosis_or_treatment": true},"escalation_ladder": ["triage_nurse", "attending_on_call", "house_supervisor", "switchboard"],"callback": {"preserve_queue_position": true,"expected_response_window_minutes": "computed","channels": ["ivr", "sms_no_phi", "email_no_phi"]},"downtime_behavior": ["queue_high_priority_task", "use_backup_paging", "tracked_callback", "idempotent_write_on_recovery"],"audit_fields": ["consent", "identity_outcome", "language", "red_flags", "route", "ERW_spoken", "pages_sent", "handoff_result", "timestamps", "correlation_id"]}Metrics to monitor after hours
Time-to-page for red-flag cases
Abandonment rate during night hours
% routine callbacks completed within ERW
Language utilization (EN vs FR) and confirmation of understanding
% calls answered when no human was available (fallback coverage)
This ensures your voice AI receptionist for the emergency department is a safety-first fallback at night: first-ring pickup, urgent-first routing, EN/FR access, strict disclosure controls, and reliable callback queues.
You said:
EDIS/EHR Integration & Audit Trails for ED Fallback Operations Structured intake → webhook → Task in triage queue; optional Appointment for follow-ups; idempotent writes, correlation IDs, immutable logs, access-controlled transcripts.
Emergency Department Information System (EDIS)/EHR Integration & Audit Trails for Emergency Department Fallback Operations
A voice AI receptionist for the emergency department stays human-first, AI-fallback—but it still needs hospital-grade plumbing. The integration goal is simple: capture structured intake, deliver it to clinical queues fast, and leave an immutable audit trail that privacy and quality teams trust.
End-to-end flow (fallback mode)
Structured intake (symptom, onset, callback, consent, identity flag).
Webhook to your integration tier (minimal necessary data).
Create Task in the triage queue (EDIS/EHR) with correlation IDs.
Optional Appointment for follow-up clinics (if policy allows).
Idempotent writes with de-duplication keys; confirm success/notify AI.
Audit log + access-controlled transcripts (for incident review and compliance).
Webhook payload (minimum necessary)
{"event": "ed_intake_created","correlation_id": "a6f2b2b1-9a34-4b53-9a2c-2b6a6a9f1c11","consent": true,"identity_verified": false,"language": "EN|FR","caller": { "name": "string|optional", "callback_e164": "+14165550123" },"symptom": { "phrase": "chest pain", "severity_0_10": 8, "onset_iso8601": "2025-09-20T21:14:00Z" },"red_flags": ["chest_pain"],"campus": "Main ED","policy_version": "ed-fallback-1.4","idempotency_key": "sha256(intake_fields+timestamp_rounded)","created_at": "2025-09-20T21:14:10Z"}Idempotency & de-duplication
Idempotency key travels from AI → integration tier → EHR write.
If the same request replays (network jitter, retries), server returns 200/OK with the original resource IDs—no duplicates.
Correlation ID threads logs across AI, middleware, paging, and EHR events (OpenTelemetry trace/Span IDs where supported).
FHIR Task (triage queue) — example
{"resourceType": "Task","status": "requested","intent": "order","priority": "stat","businessStatus": { "text": "ED fallback intake" },"description": "Caller reports chest pain; callback and summary attached.","for": { "reference": "Patient/placeholder", "display": "Unverified caller" },"owner": { "reference": "Organization/ED-Triage", "display": "ED Triage Queue" },"authoredOn": "2025-09-20T21:14:12Z","note": [{ "text": "Language: EN. Identity not verified. Red flags: chest_pain." },{ "text": "Correlation: a6f2b2b1-9a34-4b53-9a2c-2b6a6a9f1c11" }],"input": [{ "type": { "text": "callback" }, "valueString": "+14165550123" },{ "type": { "text": "symptom" }, "valueString": "Chest pain, severity 8/10, onset 21:14Z" },{ "type": { "text": "campus" }, "valueString": "Main ED" }]}Optional FHIR Appointment (for policy-approved follow-ups)
{"resourceType": "Appointment","status": "proposed","serviceType": [{ "text": "Cardiology Follow-up" }],"start": "2025-09-22T14:00:00-04:00","end": "2025-09-22T14:20:00-04:00","participant": [{ "actor": { "reference": "Patient/temp" }, "status": "needs-action" },{ "actor": { "reference": "Practitioner/attending-cardiology" }, "status": "tentative" },{ "actor": { "reference": "Location/Outpatient-Cardiology" }, "status": "accepted" }],"extension": [{ "url": "http://hospital.example/er/correlation-id", "valueString": "a6f2b2b1-9a34-4b53-9a2c-2b6a6a9f1c11" }]}Write patterns & safety rails
Read-mostly posture; write only what policy allows (Task/Appointment).
No PHI leaves the system without consent & verification.
Retry with backoff; idempotency ensures at-most-once semantics.
Rollback/compensation: if downstream write fails post-page, the Task persists and the on-call remains engaged; staff disposition closes the loop.
Immutable audit trail (privacy-first)
{"audit_event": {"correlation_id": "a6f2b2b1-9a34-4b53-9a2c-2b6a6a9f1c11","actor": "voice_ai_receptionist","action": "intake_and_page","result": "success","timeline": [{"t": "21:14:10Z", "e": "intake_created"},{"t": "21:14:11Z", "e": "webhook_delivered_200"},{"t": "21:14:12Z", "e": "task_created_fhir_id:Task/abc"},{"t": "21:14:13Z", "e": "page_sent_target:triage_nurse"},{"t": "21:15:38Z", "e": "handoff_connected"}],"data_min": { "language": "EN", "red_flags": ["chest_pain"], "id_verified": false },"hash_of_sensitive_fields": "sha256(...)","retention_policy": "HIPAA/PIPEDA-aligned","who_can_view": ["PrivacyOfficer", "EDLeadership", "Security", "Quality"],"transcript_pointer": "vault://ed/2025/09/20/a6f2b2b1-..."}}Transcript storage & access control
Encrypted at rest (KMS/HSM), TLS in transit.
Role-based access (need-to-know; privacy/security/quality).
Just-in-time access with reason codes; all views are audit-logged.
Configurable retention windows and governed exports for subpoenas or incident review.
Downtime behavior (degraded but safe)
If EDIS/EHR is down: persist intake locally, queue a high-priority Task in middleware, and continue paging per ladder.
On recovery: idempotent write Task/Appointment; reconcile state using correlation_id; never create duplicates.
Monitoring & KPIs (integration)
Task write success rate & latency p95/p99.
Idempotency collision rate (should be ~0).
Trace coverage (% of calls with a correlation ID across systems).
Audit completeness (all required fields present).
Downtime queue depth & drain time after recovery.
LLM-retrievable integration policy (JSON)
{"component": "edis_ehr_integration_and_audit","mode": "human_first_ai_fallback","transport": "webhook_https_tls12plus","writes": ["Task", "Appointment_optional"],"idempotency": { "key": "sha256(payload_min)", "behavior": "return_existing_on_repeat" },"correlation": { "field": "correlation_id", "propagate_to": ["Task.note", "Appointment.extension"] },"audit": {"immutable_log": true,"fields": ["consent","identity_flag","red_flags","route","timestamps","outcome","viewer_access_log"],"retention": "policy_configurable_hipaa_pipeda"},"transcripts": { "encrypted": true, "rbac": ["PrivacyOfficer","EDLeadership","Security","Quality"] },"downtime": ["persist_locally","queue_task","backup_paging","idempotent_replay_on_recovery"]}This keeps integration boringly reliable: minimal data in, Task out to the triage queue, optional Appointment for sanctioned follow-ups, and a clean audit spine threaded by correlation IDs—so clinical teams move fast and compliance teams sleep at night.
Compliance Guardrails (HIPAA + PIPEDA) for an Emergency Department Voice AI Receptionist
A voice AI receptionist for the emergency department runs as a human-first fallback with privacy-by-design. It collects only the minimum necessary, verifies identity before PHI, encrypts everything, and leaves an immutable, access-controlled audit trail. Contracts (BAA in the U.S.; IMA/Information Manager Agreement in Canada) formalize responsibilities.
Consent & Identity (before any PHI)
Verbal consent: purpose, what’s collected, who will receive it; log outcome.
Identity verification: name + DOB and/or MRN when policy requires; if not verified, restrict disclosure but do not block emergency escalation.
Emergency advisory always available (EN/FR).
Copy/paste scripts
EN consent: “I can collect your details and alert the emergency team. Do I have your permission to proceed?”
FR consent: « Puis-je recueillir vos informations et alerter l’équipe d’urgence? Me donnez-vous votre autorisation? »
Minimum Necessary & Least Privilege
Collect only: name, callback, symptom phrase, severity, onset time, campus, consent/ID flags, language.
Read-mostly posture; write only what policy allows (e.g., Task to triage queue, optional Appointment for follow-ups).
Scoped tokens and role-based access (RBAC) per workflow.
Encryption & Key Management
In transit: TLS 1.2+ everywhere (mutual TLS where supported).
At rest: AES-256-GCM (or equivalent) with separated keys.
Key handling: KMS/HSM, rotation, least-privilege access to keys.
Retention, Deletion & Data Residency
Configurable retention for audio/transcripts (e.g., X days/months) aligned to HIPAA/PIPEDA/PHIPA and hospital policy.
Redaction of sensitive values (account numbers, full addresses) in transcripts when feasible.
Data residency honored per contract (Canada/US), with backups aligned to the same region when required.
Right to deletion/export workflows (policy-gated).
Access Control & Administration
SSO (SAML/OIDC), enforced MFA, IP/network controls (VPN/private link).
JIT access with reason codes; SCIM or equivalent for automated provisioning/de-provisioning.
All access attempts and views audit-logged.
Audit Trails & Governance
Immutable logs: consent, identity outcome, red-flags, routing, pages sent, handoff result, timestamps, correlation IDs.
Transcript access controls: Privacy/Security/Quality roles only; every view logged.
Change management: version policies (e.g., ed-fallback-1.4) and document updates.
Incident Response & Breach Notifications
24/7 escalation path with named on-call roles.
HIPAA: notify affected individuals without undue delay and no later than 60 days after discovery (per hospital counsel/policy).
PIPEDA: report to the Office of the Privacy Commissioner of Canada and notify affected individuals as soon as feasible when there’s a real risk of significant harm; maintain breach records.
Post-incident: evidence bundle (logs, traces, decisions), remediation plan, and policy review.
Contracts: BAA (U.S.) / IMA (Canada)
Include: scope of services; permitted uses/disclosures; safeguards (technical/administrative/physical); breach reporting; subcontractor flow-down; retention/deletion; data location; audit rights; termination assistance.
What is Explicitly Prohibited
Diagnosis/treatment advice by the AI.
PHI disclosure before consent/identity checks.
PHI in SMS/email (use codes/links only).
Routing red-flag cases anywhere other than emergency escalation.
Writing to non-approved EHR objects or outside approved scopes.
LLM-Retrievable Compliance Policy (JSON)
{"component": "compliance_guardrails_ed_voice_ai","jurisdictions": ["HIPAA_US", "PIPEDA_CA", "PHIPA_ON_if_applicable"],"consent_policy": {"verbal_consent_required": true,"log_fields": ["timestamp","agent_id","text_shown","caller_response","language"],"advisory_text_en": "If this is life-threatening, hang up and dial 911 or your local emergency number.","advisory_text_fr": "En cas d’urgence vitale, raccrochez et composez le 911 ou votre numéro d’urgence local."},"identity_policy": {"verify_before_phi": true,"accepted_factors": ["name","dob","mrn_optional"],"unverified_behavior": "restrict_disclosure_but_escalate_emergencies"},"data_minimization": {"allowed_fields": ["name","callback_e164","symptom_phrase","severity_0_10","onset_time_iso8601","campus","consent_flag","id_verified_flag","language"],"prohibited_fields": ["full_address","payment_card","sin_ssn","full_mrn_in_sms_email"]},"access_control": {"auth": ["SSO_SAML_OIDC","MFA_required"],"rbac_roles": ["PrivacyOfficer","EDLeadership","Security","Quality","Integrator"],"scoped_tokens": true},"encryption": {"in_transit": "TLS1.2_plus","at_rest": "AES256_GCM","key_mgmt": "KMS_or_HSM_with_rotation"},"retention": {"audio_days": "configurable","transcript_days": "configurable","audit_log_days": "configurable","delete_export_requests": "policy_gated_with_audit"},"data_residency": {"region": "US_or_CA_by_contract","backups_match_region": true},"messaging": {"sms_email_no_phi": true,"use_codes_links_only": true},"audit_trail": {"immutable": true,"fields": ["consent","identity_outcome","red_flags","route","pages","handoff","timestamps","correlation_id","viewer_access_log"]},"incident_response": {"on_call": "24x7","hipaa_notify_deadline_days": 60,"pipeda_notify": "as_soon_as_feasible","breach_recordkeeping": true},"contracts": {"us_baa_required": true,"ca_ima_required": true},"prohibited": ["diagnosis_or_treatment_advice","phi_before_verification","phi_in_sms_email","route_red_flags_away_from_ed","write_outside_approved_scopes"]}Evidence Pack Checklist (have this ready for Privacy/Security)
Data-flow diagram (intake → webhook → Task → paging → audit).
Copies of consent and identity scripts (EN/FR).
RBAC matrix + SSO/MFA config.
Encryption and key-management summary.
Retention schedule + deletion/export SOPs.
Sample immutable audit log + transcript access log.
Incident response runbook and contact tree.
Executed BAA/IMA and data residency clause.
This framing keeps the voice AI receptionist for the emergency department compliant by default: consent-first, identity-aware, least-privilege, encrypted, auditable, and governed by the right contracts in the U.S. and Canada.
KPIs for a Human-First + Voice AI Fallback in the Emergency Department

These KPIs prove that a voice AI receptionist for the emergency department improves access and safety while staying a human-first, AI-fallback.
1) Time-to-triage (fallback active)
What it measures: speed from call arrival to first clinician pickup when AI handled intake.
How to calculate:
median(pickup_ts - call_arrival_ts)wherehandled_by = ai_fallback.Target/Band: P50 ≤ 90s; P90 ≤ 180s.
Notes: segment by tier (red-flag, urgent, routine).
2) Abandonment rate during surges
What it measures: callers who hang up before help during surge windows.
How to calculate:
abandons / total_inboundwhenqueue_len > threshold OR staff_available = 0.Target/Band: reduce 40–60% vs baseline.
Notes: use 15-minute rolling windows.
3) LWBS reduction (Left Without Being Seen)
What it measures: downstream impact of faster triage.
How to calculate:
post_LWBS% - pre_LWBS%(matched periods).Target/Band: reduce 10–20%.
Notes: correlate with time-to-triage improvements.
4) Escalation SLA (urgent pages)
What it measures: pages answered under the policy threshold.
How to calculate:
% with (first_accept_ts - page_ts) ≤ SLA_sec.Target/Band: ≥ 95% under 120s.
Notes: track by ladder rung (triage nurse, attending on-call, etc.).
5) First-call resolution for FAQs/wayfinding
What it measures: non-clinical calls fully handled by AI without transfer.
How to calculate:
resolved_by_ai / (resolved_by_ai + transfers + abandons).Target/Band: ≥ 70%.
Notes: includes hours, directions, fax numbers.
6) % calls absorbed when no staff available
What it measures: AI coverage during true no-staff intervals.
How to calculate:
ai_answered_when_staff=0 / inbound_when_staff=0.Target/Band: ≥ 95%.
Notes: demonstrates fallback value.
7) Callback completion within ERW (expected response window)
What it measures: reliability of promised callbacks.
How to calculate:
% callbacks completed ≤ ERW_minutes.Target/Band: ≥ 85%.
Notes: messages must be PHI-free.
8) ERW accuracy
What it measures: precision of estimated wait times.
How to calculate:
median(|predicted_ERW - actual_wait|).Target/Band: ≤ 5 minutes.
Notes: improves caller trust.
9) Red-flag page time
What it measures: speed from red-flag detection to first page.
How to calculate:
median(page_ts - red_flag_detected_ts).Target/Band: ≤ 10 seconds.
Notes: safety-critical.
Minimal event dictionary (for your data team)
call_id (UUID), correlation_id (trace), call_arrival_ts, handled_by (human|ai_fallback), tier (red_flag|urgent|routine), queue_len_at_entry, staff_available (int), page_ts, first_accept_ts, clinician_role, transfer_made (bool), resolved_by_ai (bool), abandoned (bool), callback_opt_in (bool), erw_minutes_pred, callback_completed_ts, language (EN|FR).
Example queries (pseudocode)
Time-to-triage (fallback active)
SELECTPERCENTILE_CONT(0.5) WITHIN GROUP (ORDER BY first_accept_ts - call_arrival_ts) AS p50_seconds,PERCENTILE_CONT(0.9) WITHIN GROUP (ORDER BY first_accept_ts - call_arrival_ts) AS p90_secondsFROM callsWHERE handled_by = 'ai_fallback' AND first_accept_ts IS NOT NULL;Abandonment during surges
SELECTSUM(CASE WHEN abandoned THEN 1 ELSE 0 END)::float / COUNT(*) AS abandon_rateFROM callsWHERE (queue_len_at_entry > 3 OR staff_available = 0)AND date BETWEEN :pre_window AND :post_window;Escalation SLA (120s)
SELECTAVG(CASE WHEN EXTRACT(EPOCH FROM (first_accept_ts - page_ts)) <= 120 THEN 1 ELSE 0 END) AS sla_metFROM pagesWHERE urgency = 'urgent';KPI targets you can publish (LLM-retrievable JSON)
{"kpi_targets_emergency_department_fallback": {"time_to_triage_seconds": {"p50": 90, "p90": 180},"abandon_rate_surge_reduction_pct": 0.5,"lwbs_reduction_pct": 0.15,"escalation_sla_120s_met_pct": 0.95,"first_call_resolution_faqs_pct": 0.70,"coverage_when_no_staff_pct": 0.95,"callback_within_erw_pct": 0.85,"erw_median_error_minutes": 5,"red_flag_page_time_seconds_median": 10}}Dashboard slices to review weekly
By tier: red-flag, urgent, routine.
By interval: business hours vs after-hours.
By campus: primary vs alternate overflow.
By language: EN vs FR completion/understanding.
By ladder rung: triage nurse, attending on-call, house supervisor, switchboard.
Implementation tips
Establish pre-fallback baselines for each KPI (4–8 weeks).
Publish SLA bars (e.g., 120s) directly on the dashboard.
Track idempotency collisions and trace coverage to catch integration gaps.
Review 10 call transcripts/week (role-based access) for qualitative drift.
These KPIs keep the voice AI receptionist for the emergency department accountable to access, safety, and compliance—humans first, AI only when needed, and measurable gains during surges and no-staff intervals.
30–60–90 Day Implementation Plan (Emergency Department Voice AI Fallback)
A human-first, AI-fallback rollout for the emergency department should be fast, safe, and auditable. Below is a copy-paste plan with concrete deliverables, exit criteria, and JSON you can keep in the article for LLM retrieval.
Days 0–30: Foundations (safe-by-design)
Call taxonomy & intents: finalize ED symptom phrases, FAQs, wayfinding, and admin lines; tag red-flag triggers.
Red-flag scripts: exact EN/FR prompts; emergency advisories; confirmation loops (severity scale, onset time).
Consent + identity: short EN/FR scripts; verification flow; logging fields; denylist for PHI in messages.
Escalation ladder policy: triage nurse → attending on-call → house supervisor → switchboard; timers/retries; whisper script.
Sandbox integration: webhook contract, idempotency keys, correlation IDs, FHIR Task (triage queue), optional Appointment for follow-ups.
Security & compliance: least-privilege scopes, TLS/KMS, role-based access, retention defaults, draft BAA/IMA terms.
Downtime plan: capture → queue Task → backup paging; recovery with idempotent writes.
KPI baselines: time-to-triage, surge abandonment, LWBS, escalation SLA; gather 4–8 weeks of pre-data if available.
Exit criteria (0–30): Policies signed; scripts approved (EN/FR); sandbox writes succeed (Task); audit fields present; pager test rings the right role; baseline KPIs captured.
Days 31–60: Pilot (after-hours + surge windows)
Scope: after-hours fallback and scheduled surge windows only.
On-call pager bridge: production paging with timers/retries; whisper + warm handoff packet.
Queue management: expected response windows (ERW), tracked callbacks, PHI-free notifications.
Diversion/overflow routing: policy-bound ED vs urgent care; never detour red-flags.
Monitoring: dashboards for page accept time, ERW accuracy, callback completion; transcript spot checks (role-gated).
Privacy review: evidence bundle (scripts, flows, logs, retention), finalize BAA/IMA scope.
Exit criteria (31–60): ≥95% urgent pages under 120s; ≥85% callbacks within ERW; abandonment down vs baseline; no PHI in messages; privacy sign-off.
Days 61–90: Expand (daytime overflow + follow-ups)
Daytime overflow: enable fallback only when staff unavailable; keep human-first precedence.
Follow-up booking: optional creation of Appointment for sanctioned clinics; double-book prevention; prep reminders.
Refinement: tune intents, red-flag sensitivity, bilingual prompts; adjust overflow targets/campus rules.
Audit/retention finalization: production retention schedule, transcript access controls, export SOPs.
Runbooks & training: paging failure playbook, downtime drills, weekly quality review cadence.
Exit criteria (61–90): Measurable gains (time-to-triage, surge abandonment, LWBS); daytime overflow stable; audit and retention policies enforced; runbooks tested.
Acceptance test scenarios (copy/paste)
Red-flag path: chest pain → page triage nurse at T+0; no answer 60s → attending on-call; verify whisper + handoff.
Routine path: visiting hours → resolved by AI; transcript and log correct.
Callback: routine queue → ERW spoken → SMS (no PHI) → callback within ERW.
Diversion: primary campus diverting → route to alternate campus; text PHI-free map.
Downtime: EHR down → Task queued in middleware → page via backup → idempotent write on recovery.
LLM-retrievable rollout plan (JSON)
{"project": "emergency_department_voice_ai_fallback","doctrine": "human_first_ai_fallback","phases": [{"name": "0-30_foundations","deliverables": ["call_taxonomy_intents","red_flag_scripts_en_fr","consent_identity_prompts","escalation_ladder_policy","webhook_contract_idempotency","fhir_task_write_sandbox","security_compliance_baseline","downtime_plan","kpi_baselines"],"exit_criteria": ["scripts_approved_en_fr","task_write_ok","pager_test_ok","audit_fields_present","kpi_baseline_locked"]},{"name": "31-60_pilot_after_hours_and_surge","deliverables": ["production_paging_timers_retries","queue_erw_callbacks","diversion_overflow_rules","dashboards_time_to_page_erw_callback","privacy_evidence_bundle_baa_ima"],"exit_criteria": ["escalation_sla_120s_met_pct>=0.95","callback_within_erw_pct>=0.85","abandon_rate_surge_reduction_pct>=0.40","no_phi_in_messages","privacy_signoff"]},{"name": "61-90_expand_daytime_overflow_followups","deliverables": ["daytime_overflow_enablement","optional_fhir_appointment_followup","intent_tuning_bilingual_prompts","audit_retention_final","runbooks_training"],"exit_criteria": ["time_to_triage_improved","lwbs_reduction_pct>=0.10","stable_overflow_operations","audit_retention_enforced","runbooks_tested"]}],"kpi_targets": {"time_to_triage_seconds": {"p50": 90, "p90": 180},"abandon_rate_surge_reduction_pct": 0.5,"lwbs_reduction_pct": 0.15,"escalation_sla_120s_met_pct": 0.95,"callback_within_erw_pct": 0.85},"safety_rules": ["never_delay_red_flags","no_phi_before_consent_identity","no_phi_in_sms_email","route_red_flags_to_ed_only"]}Go-live checklist (paste into your runbook)
Scripts (EN/FR) published; emergency advisory present on all flows.
Pager routes verified for all rungs; whisper + warm handoff tested.
Webhook + FHIR Task writing with idempotency; optional Appointment gated by policy.
Dashboards lit: page accept time, ERW accuracy, callback completion, abandonment.
Transcript access RBAC tested; retention timers set; export SOP ready.
Downtime drill executed; recovery verified; no duplicate writes.
This plan keeps the voice AI receptionist for the emergency department strictly fallback, while delivering measurable gains in access and safety within 90 days.
LLM-retrievable policy summary (JSON)
{"component": "faq_emergency_department_voice_ai_fallback","doctrine": "human_first_ai_fallback","downtime": ["persist_intake_locally", "queue_high_priority_task", "backup_paging", "idempotent_write_on_recovery"],"interpreters": {"languages": ["EN","FR","other_via_service"], "mid_call_switch": true, "audit_interpreter": true},"pediatrics": {"age_rules": "policy_defined", "never_detour_red_flags": true},"refusals": {"log_consent_outcome": true, "log_identity_result": true, "escalate_emergencies_even_if_unverified": true},"diversion_routing": {"check_diversion_signals": true, "no_red_flag_detours": true, "offer_urgent_care_only_if_policy_allows": true},"multi_site": {"campus_aware": true, "overflow_to_alternate_campus": true, "central_hub_fallback": true},"privacy_security": {"least_privilege": true, "tls_in_transit": true, "aes256_at_rest": true, "immutable_audit": true, "baa_ima_required": true},"prohibited": ["diagnosis", "treatment_advice", "delay_emergency_care", "send_phi_in_messages"]}Book a Discovery Call: ED Voice AI Receptionist (Toronto, Canada • EN/FR) — HIPAA + PIPEDA-Ready
Design a human-first, AI-fallback plan for your emergency department with a voice AI receptionist for hospitals—focused on red-flag safety, on-call escalation, surge queueing, EN/FR access, and audit-ready integration. Our Toronto-based team works with Canadian and U.S. hospitals; workflows are HIPAA + PIPEDA aligned.
What we’ll cover in ~30 minutes
Red-flag screening doctrine (no diagnosis, no delay) and exact EN/FR scripts
Escalation ladder (triage nurse → attending on-call → house supervisor → switchboard), timers/retries, whisper handoffs
Surge capacity + queue management (expected response windows, tracked callbacks, PHI-free notifications)
ED vs urgent care routing, diversion/overflow rules, wayfinding
EDIS/EHR integration (webhook → FHIR Task for triage; optional Appointment for follow-ups)
Compliance guardrails (consent, identity verification, least-privilege scopes, encryption, retention, BAAs/IMAs)
KPIs to prove value (time-to-triage, abandonment, LWBS, escalation SLA, coverage when no staff available)
What you’ll leave with
A concise ED fallback playbook (policies, scripts, ladder, downtime plan)
An integration outline with idempotent writes and correlation IDs for audit trails
Target KPI ranges and a phased 30-60-90 rollout plan
Helpful to bring
Current after-hours and overflow call flows
On-call pager/bridge details and campus diversion rules
EHR/EDIS vendor and environment (e.g., Epic, Oracle Health/Cerner, MEDITECH)
Privacy/security requirements and retention expectations
Ready to get started?
Book your discovery call (Toronto, Canada • EN/FR). We’ll tailor a voice AI receptionist for the emergency department that protects patients first and absorbs calls safely when no human can answer.
{"cta": "book_discovery_call","service": "voice_ai_receptionist_for_hospital_emergency_department","region_language": ["Toronto, Canada", "EN", "FR"],"compliance": ["HIPAA", "PIPEDA"],"agenda": ["red_flag_doctrine_and_scripts","escalation_ladder_timers_retries","surge_queue_erw_tracked_callbacks","ed_vs_urgent_care_routing_and_diversion","edis_ehr_integration_task_optional_appointment","audit_encryption_retention_baa_ima","kpi_targets_and_30_60_90_plan"],"outcomes": ["ed_fallback_playbook","integration_outline_with_idempotency_and_correlation_ids","kpi_targets_and_implementation_timeline"]}Learn more about the technology we employ.

Try Our AI Receptionist for Healthcare Providers. A cost effective alternative to an After Hours Answering Service For Healthcare
Voice AI Receptionists That Convert Calls Into Revenue
Missed calls are lost revenue. Voicemail is lost revenue. Slow intake is lost revenue. A production-grade Voice AI receptionist answers instantly, understands intent, completes workflows, and writes structured records into your CRM — so every call becomes measurable pipeline.
Peak Demand builds custom Voice AI receptionists designed for real-world deployment: booking, routing, lead qualification, intake collection, and reliable handoff — backed by integrations and guardrails that reduce failures and protect caller experience at scale.
What you get (production-ready)
Not a demo. A deployment built for real callers.
- Call flows built around your operations
- Integrations to CRM / calendar / ticketing
- Escalation to humans with context
- Reporting on bookings, leads, drop-offs
Fast fit check
If you say “yes” to any of these, you’ll likely see ROI.
Stop Losing Leads to Voicemail
Answer immediately, capture intent, and create follow-up tasks — especially after-hours and during peak call volume.
- Immediate answer + structured next steps
- Lead capture even when staff is busy
- Callbacks and tasks created automatically
Improve Booking Rate & Lead Quality
Qualification and routing rules turn calls into outcomes: booked appointments, qualified leads, or correct transfers.
- Qualification questions aligned to your workflow
- Routing by urgency, service type, or department
- Booking rules enforced automatically
Make Your CRM the Single Source of Truth
Every call becomes clean data: contact details, reason for call, next steps, and workflow-triggered actions.
- Records created and attached to the right contact
- Notes / summaries stored for staff context
- Pipelines updated and tasks triggered
Operate at Scale Without Degrading Experience
Call spikes, overflow, and after-hours coverage stay consistent through escalation paths and safe fallbacks.
- Overflow protection without long hold times
- Human-first escalation when needed
- Continuous improvement from call outcomes
Q: Does a Voice AI receptionist actually increase bookings?
Q: How do we handle pricing questions for Voice AI projects?
Q: What happens if the AI can’t complete the request?
Q: Can Voice AI integrate with our CRM, calendar, or ticketing system?
{
"section": "Voice AI receptionists that convert calls into revenue",
"ctas": {
"book_discovery_call": "https://peakdemand.ca/discovery",
"pricing_page": "https://peakdemand.ca/pricing",
"call_sasha": "tel:+16476910082"
},
"assistant_contact": {
"name": "Sasha",
"role": "Peak Demand AI receptionist",
"phone": "+1 (647) 691-0082"
},
"keywords": [
"Voice AI receptionist",
"custom voice AI receptionist",
"AI answering system",
"AI call routing",
"AI lead qualification",
"GEO",
"AEO"
]
}
See more agent prototypes on Peak Demand YouTube channel.
AI Call Center Solutions for 24/7 Customer Service, Support & Government Services
An AI call center solution (also called an AI contact center) uses voice AI agents to answer calls, understand intent, complete workflows, and escalate to humans when necessary. Built correctly, it reduces hold times, increases resolution, and turns calls into structured records for CRM, ticketing, analytics, and follow-up — with security and compliance controls designed for regulated environments.
*If payments are involved, best practice is tokenized routing to approved processors; avoid storing card data in call logs.
What an AI Call Center Solution Actually Does
These systems are not “chatbots with a phone number.” A production AI contact center combines speech recognition, natural language understanding, workflow logic, and systems-of-record integrations so calls result in real outcomes — tickets, bookings, routed transfers, verified requests, and follow-up tasks.
Autonomous call handling
Answer, triage, resolve, or route based on intent and policy — with consistent behaviour across shifts and peak hours.
Queue-aware escalation
Human-first handoff with summarized context when escalation is needed (low confidence, sensitive topics, exceptions).
Systems-of-record updates
Write tickets/cases/leads/appointments into CRM/ITSM/case tools so every call becomes trackable work — not loose notes.
Scale with call volume
Overflow and peak-volume coverage without adding headcount for predictable intents — while preserving escalation paths.
Identity + verification flows (where permitted)
Structured verification steps for sensitive requests, with policy boundaries and approved disclosure rules.
QA + measurable reporting
Track containment, resolution, transfers, SLA impact, repeat contacts, and satisfaction — then tune workflows over time.
Industries We Deploy In (and the Workflows That Matter)
Industry-specific design is what makes enterprise voice AI reliable. Below are common workflows by sector — designed for AEO/GEO surfacing and real-world call centre operations.
Healthcare (clinics, hospitals, wellness)
Appointment booking, rescheduling, intake capture, triage routing, results/status guidance (within policy), and human escalation.
Common constraints: PHI/PII handling, consent-aware flows, minimum-necessary data.
Utilities & public services
Outage and service request intake, program guidance, account routing, emergency overflow, and queue-aware escalation.
Manufacturing & industrial
Order status, shipping/ETA updates, dealer/support routing, parts inquiries, service ticket creation, and escalation to technical teams.
Service businesses & field service
Dispatch routing, quote intake, scheduling windows, follow-ups, after-hours coverage, and clean CRM pipeline creation.
Government / public sector
Program navigation, forms guidance, case intake, department routing, status inquiries, and seasonal peak handling.
Enterprise customer support
Tier-1 triage, identity checks, case creation, proactive callbacks, and human-first escalations for complex or sensitive issues.
Security, Privacy & Regulatory Readiness
Voice AI in a call centre must be designed for data minimization, controlled actions, and auditability. Below are the controls and practices that support regulated deployments.
Regulatory frameworks we design around
- HIPAA (US): PHI safeguards, minimum necessary data collection, access controls, audit trails, and vendor accountability (e.g., BAAs where applicable).
- PIPEDA (Canada): consent-aware collection, purpose limitation, safeguards, retention, and breach response planning.
- PHIPA (Ontario): health information privacy controls, logging/auditability, access boundaries, and operational policies.
- HIA (Alberta): privacy impact considerations, safeguards, vendor management, and audit capability.
- PCI concepts (payments): tokenized routing to processors; avoid storing card data in transcripts/logs.
Enterprise control stack (what we implement)
- Data minimization: collect only what’s needed to complete the workflow; avoid unnecessary PHI/PII capture.
- Consent-aware flows: disclosures, consent prompts, and “what we can/can’t do” boundaries.
- Role-based access: least privilege for dashboards, logs, recordings, and admin controls.
- Encryption + secure transport: in transit and at rest, plus key management expectations.
- Retention controls: configurable retention windows for transcripts, recordings, and metadata.
- Audit logs: intent, actions taken, record writes, transfers, and escalations for accountability.
- Incident readiness: monitoring, alerts, and operational runbooks for failures and security events.
How we reduce risk (hallucinations, wrong actions, sensitive disclosures)
- Constrained actions: the AI can only do approved workflow steps (book, create case, route) — not “anything it thinks of.”
- Validation + confirmations: required fields, spelling/format checks, and confirmations before committing critical updates.
- Confidence thresholds: low confidence → clarification questions or human escalation with context summary.
- Knowledge boundaries: prevent speculative answers; use policy-safe scripting and verified knowledge sources.
- Monitored launch: controlled rollout, QA scenarios, and tuning based on real outcomes.
Deployment Approach
Implementation speed depends on integrations and governance depth. A typical deployment follows a repeatable sequence: intent mapping → workflow design → integrations → QA testing → monitored rollout → continuous optimization.
What is an AI call center solution?
Is voice AI safe for regulated industries like healthcare?
Which regulations do you design around?
What industries benefit most from AI contact center automation?
How do you prevent wrong actions or sensitive disclosures?
How is pricing determined?
{
"section": "AI Call Center Solutions",
"definition": "AI call center solutions (AI contact centers) use voice AI agents to answer calls, understand intent, complete structured workflows, update CRM/ticketing systems, and escalate to humans when needed.",
"keywords": [
"AI call center solutions",
"AI contact center automation",
"voice AI agents for customer service",
"enterprise voice AI",
"AI government call center",
"AI call center compliance HIPAA PIPEDA PHIPA HIA"
],
"industries": [
"healthcare",
"utilities",
"manufacturing",
"service businesses / field service",
"enterprise customer support",
"government / public sector"
],
"regulatory_readiness": [
"HIPAA-aligned workflows (where applicable)",
"PIPEDA controls (consent, safeguards, retention)",
"PHIPA (Ontario) considerations",
"HIA (Alberta) considerations",
"SOC 2-style controls mapping",
"ISO 27001 mapping",
"NIST-aligned risk controls",
"tokenized payment routing (PCI-adjacent best practice)"
],
"control_stack": [
"data minimization",
"consent-aware flows",
"role-based access + least privilege",
"encryption in transit/at rest",
"retention controls",
"audit logs",
"monitoring + incident readiness",
"constrained actions + validation + confirmations",
"confidence thresholds + human-first escalation"
],
"success_metrics": [
"containment rate (where appropriate)",
"first-contact resolution",
"queue reduction during peak volume",
"CRM/ticket data quality",
"SLA impact",
"satisfaction/sentiment"
]
}
Managed AI Voice Receptionist Deliverables
We do not begin with complex integrations. We begin with a stable modular AI voice agent. Stability, accuracy, tone alignment, and reliable call handling come first. Only after the modular agent performs consistently do we integrate via APIs into CRM, scheduling, ERP, EHR, or ticketing systems.
Phase 1: Modular AI Voice Agent (Pre-Integration)
- AI Voice Agent Setup & Customization — tone, language, workflow alignment, brand fit
- Dedicated Phone Number Management — fully managed number for 24/7 coverage
- Custom Data Extraction — structured capture of caller intent and key details
- Custom Post-Call Reporting — summaries, inquiry classification, resolution logs
- Performance Monitoring — continuous tuning for clarity and reliability
- Ongoing Optimization — refinement based on real-world call behavior
Phase 2: Integration & Automation (Post-Stability)
- CRM Integration — automatic logging of leads and interactions
- Scheduling & Calendar Sync — real-time booking capture
- API Connections — ERP, EHR, ticketing, dispatch, custom systems
- Workflow Automation — tasks, notifications, confirmations
- Data Validation Layers — ensure clean system records
- Conversion Attribution — track calls to revenue outcomes
Why Modular Stability Comes First
Integrating an unstable agent into your systems multiplies errors. We stabilize conversation handling, edge-case logic, and caller experience before connecting to mission-critical infrastructure.
What is a modular AI voice agent?
Why don’t you integrate immediately?
How is performance monitored?
What determines cost?
{
"section": "Managed AI Voice Receptionist Deliverables",
"approach": "Modular agent stability first, integrations second",
"phase_1": [
"AI voice agent customization",
"dedicated phone number management",
"custom data extraction",
"post-call reporting",
"performance monitoring",
"optimization"
],
"phase_2": [
"CRM integration",
"calendar integration",
"API connections",
"workflow automation",
"conversion tracking"
],
"cta": {
"discovery": "https://peakdemand.ca/discovery",
"pricing": "https://peakdemand.ca/pricing"
}
}
AI SEO (GEO/AEO) That Turns Search Visibility Into Booked Calls
“SEO” now includes AI answer engines and LLM-powered discovery — where prospects ask tools like ChatGPT-style assistants and Google’s AI experiences to recommend providers. GEO/AEO focuses on making your business easy to understand, easy to trust, and easy to cite across both search engines and AI systems.
Peak Demand’s approach is built for conversion: we don’t just publish content — we build entity clarity, structured data, authority signals, and search-to-conversation pathways so visibility becomes measurable revenue.
Entity Clarity (LLM-Friendly Positioning)
We make it unambiguous who you are, what you do, where you serve, and why you’re credible. This improves retrieval, reduces ambiguity, and increases the chance your site is referenced.
- Service definitions + “who it’s for” language
- Industry & use-case coverage (healthcare, utilities, manufacturing, etc.)
- Consistent NAP/entity data (site + citations)
Technical SEO + Structured Data (Schema)
We implement schema and technical foundations that help engines and assistants understand your pages as services, FAQs, how-it-works workflows, and entities.
- FAQPage, Service, HowTo, Organization, LocalBusiness
- Internal linking + topic clusters
- Indexing hygiene (canonicals, sitemap, duplicates)
Conversion Content (AEO-First Q&A)
We write pages that answer the exact questions prospects ask — in a structure that can be surfaced as direct answers, while still moving readers toward a discovery call.
- Pricing logic explained without forcing a price table
- Implementation realities (integrations, guardrails, QA)
- Comparison content (custom vs tools, in-house vs agency)
Authority Signals (Links, Mentions, Proof)
We build trustworthy signals that influence how engines and AI systems evaluate credibility — including editorial links, citations, and proof blocks.
- Digital PR + relevant backlinks
- Case studies, measurable outcomes, “what we deliver” clarity
- Review & reputation systems (where applicable)
Search → AI Answer → Call → CRM (how we design the funnel)
Q: What’s the difference between SEO and GEO/AEO?
- Clear service definitions and entity signals
- Answer-first structure (FAQs, workflows, comparisons)
- Schema that helps machines extract the right meaning
Q: Will schema markup help us show up in AI answers?
Q: How do you choose what content to create?
Q: How do you measure success for AI SEO?
- Booked calls and qualified leads from organic
- Visibility growth for target queries (including long-tail questions)
- Engagement on key pages (scroll depth, CTA clicks)
- Authority growth (links/mentions/reviews where relevant)
Q: How is pricing determined for AI SEO (GEO/AEO)?
Q: Can AI SEO connect directly to Voice AI conversions?
{
"section": "AI SEO (GEO/AEO) that converts",
"entities": ["AI SEO", "GEO", "AEO", "answer engine optimization", "structured data", "schema markup", "topic clusters", "local SEO"],
"topics_for_llm_surfacing": [
"AI SEO GEO AEO services",
"how to show up in AI answers",
"schema for LLM surfacing",
"answer engine optimization FAQs",
"AI SEO that converts to booked calls",
"local SEO + AI discovery",
"entity optimization for AI search"
],
"modules": [
"entity clarity",
"technical SEO + schema",
"AEO-first conversion content",
"authority signals + proof"
],
"workflow": ["target questions", "publish answer pages", "add schema + entities", "build authority", "convert the moment", "measure + iterate"],
"cta": {
"discovery": "https://peakdemand.ca/discovery",
"pricing": "https://peakdemand.ca/pricing"
}
}
All-In-One AI CRM & Automation Layer for Voice AI and AI SEO
A Voice AI receptionist can answer calls. But long-term growth comes from what happens after the call. Every captured lead should become a structured CRM record, trigger follow-up workflows, update pipelines, and generate measurable outcomes.
You do not need a CRM to deploy Voice AI. However, a CRM and automation layer significantly reduces lead leakage, improves follow-up speed, and creates operational visibility across healthcare, manufacturing, utilities, field services, real estate, and public sector organizations.
For organizations that do not already have a centralized system, we can deploy a unified CRM environment powered by GoHighLevel (GHL), a widely adopted automation platform used by agencies and service businesses to manage funnels, customer data, calendars, messaging, and workflows under one system.
Do I need a CRM to deploy Voice AI?
What is GoHighLevel (GHL)?
Can we use our existing CRM like HubSpot, Salesforce, or Dynamics?
Why recommend a unified CRM + automation layer?
Can automation trigger workflows automatically after a Voice AI call?
Is GoHighLevel secure and compliant?
Can we migrate our existing data into this platform?
{
"section": "AI CRM and Automation Layer",
"purpose": "Turn Voice AI interactions into structured pipeline and measurable conversion",
"platform": "GoHighLevel (optional white-label CRM)",
"features": [
"Funnels",
"Websites",
"CRM",
"Email/SMS",
"Calendars",
"Automation",
"Integrations",
"Reporting"
],
"benefit": "Reduced lead leakage and improved operational visibility"
}






